Chicago's Advanced CGM Supplies
Get Medicare-covered diabetes management supplies delivered directly to your home across Chicagoland & beyond.

Simplifying CGM Access: Local, Insurance-Covered Care
Skip Pharmacy Stress With The Hayat DME Advantage
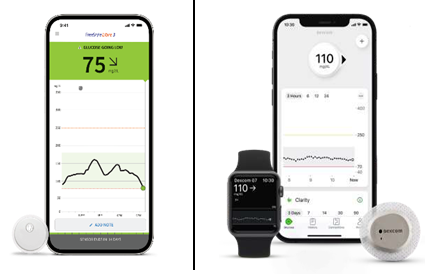
As Chicago’s trusted local provider of durable medical equipment (DME) and home care equipment, Hayat has been dedicated to streamlining patient access to advanced technology since 2019. We specialize in simplifying the process for Medicare patients in the Chicago, IL area to receive the latest Continuous Glucose Monitors (CGM), including the Dexcom G7 and FreeStyle Libre.
We understand that effective diabetes management depends on constant glucose monitoring, and dealing with pharmacy benefits can be complicated and costly. As a specialized DME provider, Hayat eliminates the stress by navigating insurance, working directly with your Illinois physician’s office, and ensuring your diabetic supplies are covered under your DME benefit. Our goal is to make sure your receiver and sensors are delivered promptly to your home.
The Hayat Advantage: Seamless Service
• Timely Re-Order Assurance: Our team proactively contacts you 5–7 days before your sensor expires to process your re-order, ensuring your glucose monitoring is constant and reliable.
• Local Physician Partnership: We work closely with your local care team to manage paperwork, making the process faster and easier than navigating complex pharmacy channels.
• Expert Setup & Support: As a dedicated home care equipment provider, we ensure you have the support needed for successful CGM use.

Traditional Fax Order (708) 422-5966
 Required Documentation (For Quick Processing)
Required Documentation (For Quick Processing)
To minimize delays in delivery, please ensure your physician provides the following documents:
- Patient demographic sheet and copies of both insurance cards.
- Signed Detailed Written Order (DWO).
Most Recent Office Notes (must be within six months)
that verify the eligibility criteria listed below:
Medicare CGM Qualification Criteria (Detail)
Diagnosis of Diabetis Mellitus
Beneficiary’s treating practitioner has concluded that the beneficiary (or beneficiary’s caregiver)
has sufficient training using the CGM prescribed as evidenced by providing a prescription.
CGM is prescribed in accordance with its FDA indications for use
Beneficiary for whom a CGM is being prescribed, to improve glycemic control, meets at least one of the criteria below:
- The beneficiary is insulin-treated; or,
- The beneficiary has a history of problematic hypoglycemia with documentation of at least one of the following:
- Recurrent (more than one) level 2 hypoglycemic events (glucose <54mg/dl (3.0mmol/L)) that persist despite multiple (more than one) attempts to adjust medication(s) and/or modify the diabetes treatment plan; or,
- A history of one level 3 hypoglycemic event (glucose <54mg/dl (3.0mmol/L)) characterized by altered mental and/or physical state requiring third-party assistance for treatment of hypoglycemia
Within six (6) months prior to ordering the CGM, the treating practitioner has an in-person or Medicare-approved telehealth visit with the beneficiary to evaluate their diabetes control and determine that criteria (1-4) above are met.
PATIENT WILL BE CONTACTED WITHIN
24-48 HOURS TO CONFIRM ORDER AND
SETUP DELIVERY VIA MAIL ORDER